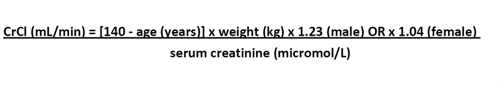Skip to main content
Announcements and latest updates
Signs and symptoms
- Common symptoms include malaise, weakness, anorexia, thirst, nausea, constipation and polyuria.
- Severe symptoms include nausea, vomiting, ileus, delirium, seizures, drowsiness and coma.
- Pain can be precipitated or exacerbated by hypercalcaemia.
- Onset of symptoms raising clinical suspicion should be investigated. Bloods should be checked for urea and electrolytes (U&Es), estimated glomerular filtration rate (eGFR), liver function tests (LFTs) and calcium.
eGFR Caution Note:
- The use of creatinine-based equations will lead to an overestimation of the Creatinine Clearance (CrCl) and eGFR in individuals with reduced body size or muscle mass, e.g. frail, elderly, critically ill or patients with cancer or muscle wasting diseases. The absolute GFR or CrCl calculated by the Cockcroft & Gault formula should be used to adjust drug dosages in patients at extremes of body weight (BMI <18.5kg/m2 or >30kg/m2). If using C&G for these patients it may be necessary to base the calculation on ideal body weight or adjusted body weight, see below.
Estimation of creatinine clearance (CrCl)
- The following 'Cockcroft Gault' equation can be used to estimate creatinine clearance (CrCl).
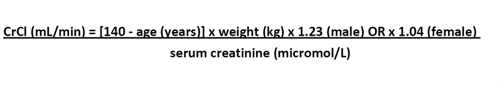
Caution
- Use actual body weight or maximum body weight whichever is lower. Refer to this table.
- In patients with low creatinine (<60 micromol/L), use 60 micromol/L.
- Use of estimated glomerular filtration rate (eGFR) is not recommended.
Points to consider prior to treatment
- First episode or long interval since previous episode.
- Patient reports good quality of life prior to episode.
- Multidisciplinary team expectation is that treatment will have durable effect.
- Patient is willing and able to have intravenous treatment and blood tests.
- Treatment may not be appropriate in a dying patient at the end of life – seek advice.